By GREGORY ZELLER //
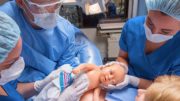
An innovative “bridge” linking South Shore University Hospital to a groundbreaking breastmilk clinic is delivering human milk to premature babies whose mothers might not be ready to produce.
 Leveraging the science-supported principle that human milk is healthier for infants than mass-produced baby formula, the Bay Shore-based Northwell Health hospital has officially launched a donor breastmilk program targeting infants in its Neonatal Intensive Care Unit – specifically, babies born around 34 weeks of pregnancy or earlier.
Leveraging the science-supported principle that human milk is healthier for infants than mass-produced baby formula, the Bay Shore-based Northwell Health hospital has officially launched a donor breastmilk program targeting infants in its Neonatal Intensive Care Unit – specifically, babies born around 34 weeks of pregnancy or earlier.
At that stage of pregnancy (about 8 months, give or take), many mothers are not physiologically ready to produce breastmilk. The bridge – part of a broader Northwell Health effort that includes other birthing hospitals within the sprawling health system – aims to bring in donor milk to keep premature babies fed and nourished while avoiding baby formula, which is often processed from cow’s milk and can be more difficult to digest for early-stage infants.
Considered “liquid gold” by many obstetricians, pediatricians and neonatologists (pediatricians specially trained to care for newborns with injuries or illnesses, including preterm deliveries), human breastmilk can be especially important to “preemies” that arrive three to five weeks before they’re due.

Wendi Andria: Essential support for premature babies.
While the U.S. Department of Health and Human Services reports “no conclusive evidence that preterm infant formula” causes necrotizing enterocolitis – a life-threatening intestinal disease often afflicting preterm babies – the department also notes “strong evidence that human milk is protective against NEC.”
The ultimate conclusion, according to HHS, is that it’s “the absence of human milk – rather than the exposure to formula – that is associated with an increase in the risk of NEC.”
Wendi Andria, a registered nurse certified in inpatient obstetrics and SSUH’s clinical program manager for lactation services, called donor breastmilk an “invaluable support for preterm infants, particularly when a mother’s milk is delayed or limited.”
“Our donor breastmilk program ensures that every infant in the NICU has access to these essential benefits, giving parents peace of mind as they navigate the challenges of early life in the NICU,” Andria added.
South Shore University Hospital partners directly with the Valhalla-based New York Milk Bank, a nonprofit clinical clearinghouse that sources human breastmilk from thoroughly screened donors before pasteurizing it and freezing it for safe storage and delivery. The milk arrives at SSUH on an order-by-order basis, ready to be thawed and fed to waiting preemies.
Launched in 2016, the New York Milk Bank claims to have saved the lives of 1.8 million premature babies born around the state – making it the perfect partner for SSUH’s ambitious donor breastmilk program, according to hospital President Irene Macyk, who’s both a PhD and an RN.

Got milk?: The New York Milk Bank does, and 1.8 million preemies (and counting) are thankful for that.
“The launch of our donor breastmilk program underscores SSUH’s commitment to providing the highest level of care for our community’s vulnerable newborns,” Macyk said in a statement. “We’re proud to offer this service to our community and to give every child in our NICU the best possible start.”
And new parents like Stephanie and Kyle Devine are thrilled to receive it. When their son, Benjamin, arrived on Sept. 18, he was more than seven weeks early – a premature delivery traced to Stephanie’s severe preeclampsia, a dangerous medical condition marked by extremely high blood pressure in expectant mothers and other life-threatening symptoms in both mother and baby.
Benjamin weighed just 3 pounds, 2 ounces when he met the world – an unexpected and scary reality for the Devine family.
“Having our baby in the NICU was one of the most overwhelming experiences,” Stephanie noted. “I wasn’t producing milk right away.”
Enter the new donor breastmilk program, which cut through the hectic noise and “made so much sense,” the new mom added. Flash forward eight weeks, and Benjamin – now weighing more than 6 pounds – is home and healthy.
“It felt incredibly reassuring to know he was getting all the nutrients he needed from another mother’s milk,” Stephanie said. “It was a bit of a no-brainer.”