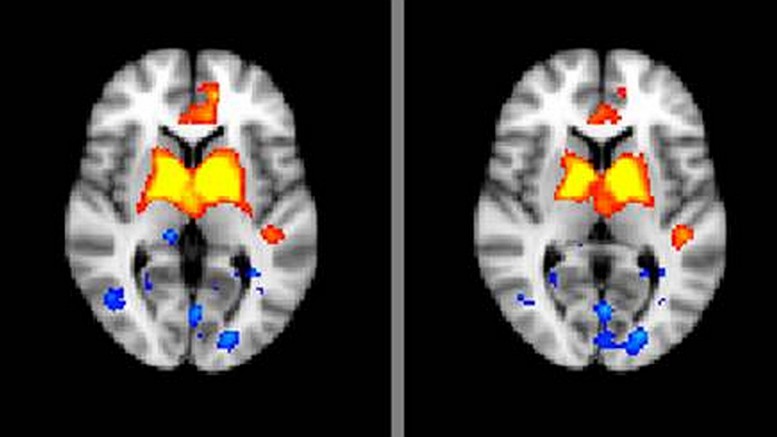
By GREGORY ZELLER // This is your brain. This is your brain on antipsychotic medications. Any questions?
Investigators at the Feinstein Institute for Medical Research, the R&D wing of the North Shore-LIJ Health System, have plenty. Among them: Can doctors use brain scans to predict how patients will respond to antipsychotic medications – even before medications are prescribed?
Such predictability would allow providers to fine-tune prescribed meds and doses, a potentially enormous innovation in the multi-billion-dollar sphere of schizophrenia, bipolar disorder and related psychiatric conditions.
According to Feinstein researchers, the answer is maybe. A research team led by Drs. Deepak Sarpal and Miklos Argyelan – attending physicians at North Shore-LIJ’s Zucker Hillside Hospital in Glen Oaks – has determined that certain brain scans can be used to create a baseline index that might help physicians accurately predict patient responses to various medications.
A study chronicling the work was published in August by the American Journal of Psychiatry. The study focused on patients suffering from first-episode schizophrenia – generally regarded as more responsive to antipsychotic compounds than multiple-episode patients – and involved fMRI brain scans prior to the prescription or ingestion of conventional antipsychotic medications.
As opposed to traditional magnetic-resonance imaging, which gives detailed snapshots of the brain’s physical structure, fMRIs – for “functional” MRI – illustrate the parts of the brain that are receiving oxygen or are otherwise active. “This gives us a better idea how the structures are functioning and what sort of activity is going on within them,” Sarpal noted.
Researchers scanned schizophrenia patients in a resting state – lying still with their eyes closed for five minutes, substantially reducing brain functions – to create the baseline. Sarpal and his team focused specifically on the striatum, a central region of the brain often implicated in schizophrenia cases.
The patients in the “discovery cohort” were subsequently prescribed one of two mainstream antipsychotic medications as part of a separate National Institutes of Health study. After 12 weeks of medications, the research team compared individual patients’ progress to the baseline brain activity.
“We used that information to extract functional connections that were predictive of response,” Sarpal said. “Once we found those functional connections, we aggregated them and came up with the Striatal Connectivity Index.”
The SCI is what researchers hope will eventually “predict the ultimate response” to medications, Sarpal noted – basically, “predicting who will respond to medications and who won’t.”
While it sounds fairly simple, the Feinstein scientists actually covered plenty of new ground. According to Sarpal, the study marked the first time researchers used fMRIs for this purpose.
“What makes this unique is we’re testing patients before they’re treated,” he said. “Our goal wasn’t to see what was going on inside there, but to see how we can apply this data to clinical practices.”
After crunching the discovery cohort’s data, researchers were able to determine “very high sensitivity and specificity” that “significantly separated responders from non-responders,” Sarpal added.
They then applied the SCI to a “replication group” including patients suffering more advanced stages than first-episode schizophrenia, many of whom had been previously medicated. It’s unclear how those prior prescriptions affected the outcome, Sarpal said, but researchers were again able to predict “significant separation” between responders and non-responders.
“We see it as a strength that they had been treated and had a variety of different diagnoses,” the lead researcher noted. “To us, it means this measure may be generalizable to a wider population of psychosis patients.”
While the results from the replication group are extremely encouraging, the science is still not solid enough “to utilize it clinically,” according to Sarpal. More testing is needed, he said, allowing researchers to “refine our index to the point where we can say something more reliable about … what medications patients should or shouldn’t take.”
For a multi-billion-dollar industry in which prescriptions set the pace, the implications are huge. In March, Forbes noted that “stagnant science” forced major players like GlaxoSmithKline and Bristol-Myers Squibb out of the neuroscience game over the last half-decade, but advances in genetic sequencing and new DNA-editing technologies have reinvigorated the field.
In 2014, investors poured some $3.3 billion into firms developing drugs to treat psychiatric illnesses – more than in any year since 2004, according to Forbes.
New antipsychotic medications are coming, but medical science still doesn’t have “biomarkers or lab tests that can guide doctors on how we select our medications, or how patients will respond to the medications they’re given,” Sarpal said.
That makes the SCI a potentially valuable tool for drug-makers, healthcare providers and patients alike. And while the Feinstein team’s research is “still in its infancy,” it looks “very promising,” according to Sarpal.
“The scenario now is clinicians will use trial-and-error – sometimes, a very lengthy trial – to see if patients will respond to treatment,” he said. “This often increases the burden on patients and their families, and sometimes creates a lot of doubt about the use of certain medications.
“This brings us one step closer to precision medicine,” Sarpal added. “It’s going to take more replication and further refinement, and it’s hard to put a timeframe on that, but I would say in the near future – perhaps a couple of years – this sort of method could be applied regularly.”