By TERRY LYNAM //
The mental health of America’s kids was a concern long before COVID-19 upended society, so no one should be surprised by a new government study showing that three out of four high school students experienced a potentially traumatic event during the pandemic – or that those events contributed to emotional distress, including suicidal behaviors.
 The survey of 4,390 U.S. high schoolers, conducted in 2021 by the U.S. Centers for Disease Control & Prevention and released Oct. 14, found that 31.1 percent reported poor mental health during the pandemic, with 19.9 percent considering (and 9 percent attempting) suicide in the prior year.
The survey of 4,390 U.S. high schoolers, conducted in 2021 by the U.S. Centers for Disease Control & Prevention and released Oct. 14, found that 31.1 percent reported poor mental health during the pandemic, with 19.9 percent considering (and 9 percent attempting) suicide in the prior year.
Nearly three-quarters of respondents reported at least one traumatic experience, including physical/emotional abuse, a parent or caregiver losing a job, sexual/dating violence, food insecurity and online bullying. And one in 13 adolescents reported four or more “adverse childhood experiences” during COVID, significantly increasing their suicide risks.
The good news, at least on Long Island, is that schools are doing their part to respond to the youth mental-health crisis declared last year by the American Academy of Pediatrics, the American Academy of Child & Adolescent Psychiatry, the Children’s Hospital Association and the U.S. surgeon general.

Terry Lynam: Youth brigade.
Thirty-eight Long Island districts – encompassing 249 schools and 178,000 students – are working with Northwell Health’s Cohen Children’s Medical Center and South Oaks Hospital through a mental-health partnership aimed at providing early intervention and trauma-informed care to kids struggling with depression, anxiety, suicidality, eating disorders, substance abuse, attention deficit hyperactivity disorder, anger-management issues and other behavioral-health problems.
One out of five U.S. children today have been diagnosed with a mental-health disorder, and suicide is the second-leading cause of death for adolescents and children as young as age 10. Particularly frustrating for parents is that a shortage of adolescent mental-health specialists can make it difficult to find timely help.
To their credit, Northwell and their school partners got out in front of this issue five years ago, before the pandemic added fuel to the simmering crisis. Cohen Children’s opened a pediatric behavioral health urgent-care center on its New Hyde Park campus in 2017. South Oaks, an Amityville-based psychiatric hospital, began working with Suffolk County school districts in 2018, sending psychiatrists into the schools to assess students, meet with parents and make recommendations.
Cohen Children’s then opened the first of its three Pediatric Behavioral Health Centers in Rockville Centre in January 2020 (about a month before the pandemic struck), first partnering with five school districts before expanding to nine southern Nassau districts the following year. Cohen opened a second Pediatric Behavioral Health Center in Mineola in 2021, which partners with 11 school districts in central and northern Nassau, and in September opened another in Commack, serving six Suffolk districts.
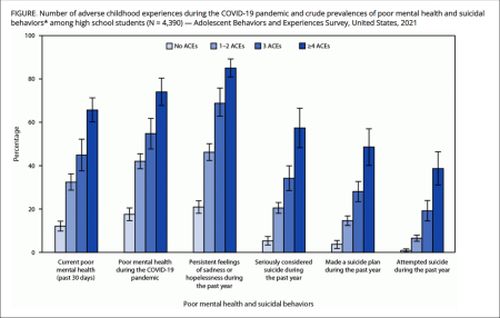
Downward trend: The pandemic has taken a mental-health toll on young people. (Source: U.S. Centers for Disease Control and Prevention)
“We used to have difficulty connecting kids with care,” notes Helen Kanellopoulos, assistant superintendent of pupil personnel services and special education for Freeport Public Schools, where 260 of the district’s 7,100 students were referred to the Rockville Centre Behavior Health Center in 2021.
Previously, Kanellopoulos says, students waited six months to get an appointment with a psychiatrist, psychologist or clinical social worker – and those in imminent crisis had to go to hospital emergency departments. Now center staff meet biweekly with the assistant superintendent and her team to “discuss what’s going on and what we are seeing,” including any new developments that may be stressing out students.
“The program has been a tremendous asset for not only us as a school, but for parents,” Kanellopoulos adds. “It has given us a layer of support that we didn’t have previously.”
Over the past two-and-a-half years, the three centers have evaluated more than 3,500 combined students, with most of those visits occurring in the past year as demand has grown and the number of participating schools have increased.

Vera Feuer: Innovation in action.
“This type of crisis access for schools does not really exist anywhere else,” notes Vera Feuer, assistant vice president of school mental health and director of emergency psychiatry at Cohen Children’s.
Feuer says she’s been hearing from many other healthcare providers throughout the state and country interested in learning more about this unique care-delivery model. According to the assistant VP, the Rockville Centre and Mineola programs alone have reduced mental-health crisis referrals from the participating schools to Cohen’s Pediatric Emergency Department by 60 percent.
“It is an innovative program and seems to be working,” she adds. “The schools are responding very positively.
“They really just want more services and we’re trying to meet the needs.”
While COVID’s social and educational disruptions have certainly had an adverse effect on young people, Feuer believes the pandemic led to more open, honest discussions about mental health – including new state-mandated mental-health education protocols that have also helped raise awareness among students.
“It’s the silver lining of the pandemic,” she says. “The conversation around mental health over the past two years has shifted – it has become a little bit more destigmatized, so more people are reaching out for help.”
Terry Lynam is a communications consultant and former senior vice president/chief public relations officer for Northwell Health.







Great column, Terry. As a public relations consultant who has worked with mental health non-profits over the years, I understand that “mental health is health,” plain and simple. We need to shed the shame and stigma associated with seeking mental health services. And with Northwell’s help — and that of other organizations such as the Ronkonkoma-based Association for Mental Health and Wellness — we’re getting there. Thanks for shining a light on this most important topic.