By TERRY LYNAM //
With COVID-19 claiming more than 1 million U.S. lives in the past 36 months and drug overdoses killing another 107,000 Americans in 2021 alone, it’s no wonder the national average life expectancy dropped again last year – to age 76, the lowest mark since 1996.
 What’s stunning, according to a new report released last week by the U.S. Centers for Disease Control & Prevention’s National Center for Health Statistics, is the historic nature of the decline. The drop of almost three life-expectancy years – from 78.8 in 2019 to 76.1 last year – represented the sharpest two-year decline in more than 100 years.
What’s stunning, according to a new report released last week by the U.S. Centers for Disease Control & Prevention’s National Center for Health Statistics, is the historic nature of the decline. The drop of almost three life-expectancy years – from 78.8 in 2019 to 76.1 last year – represented the sharpest two-year decline in more than 100 years.
You have to go back to the American Civil War – when the loss of an estimated 750,000 Americans decreased average U.S. life expectancy from 39.4 (1860) to 35.1 (1865) – to find a more dramatic decrease. Not even the one-two punch of World War I, which killed about 117,000 U.S. soldiers between 1917 and 1918, and the 1918-1919 influenza pandemic, which killed about 675,000 Americans, comes close: Between 1915 and 1920, average life expectancy declined less than a year, from 54.1 to 53.2.
The approximately 460,000 U.S. deaths from COVID in 2021 were responsible for half of the roughly 1-year drop in life expectancy between 2020 to 2021. Accidental fatalities attributed to motor-vehicle crashes, drownings, falls and drug overdoses – officially categorized by public health officials as “poisonings” – were the second-largest factor, killing more than 200,000 Americans last year.

Terry Lynam: Dead ringer.
These so-called “unintentional injuries” are the leading cause of death among Americans ages 1 to 44, and fatalities within that age group have jumped by about 33 percent over the past five years – driven primarily by drug overdoses traced to the powerful synthetic opioid fentanyl.
Heart disease and cancer are still the top two killers of Americans, claiming nearly 1.3 million lives last year. But those numbers have been declining steadily for many years – the clear culprits over the past two years are COVID and opioids.
No populations have been hit harder than American Indians and Alaskan natives, underscoring the severity of the chronic illnesses and healthcare disparities that have plagued them for decades. Their combined life expectancy dropped 1.9 years between 2020 and 2021 and fell an astounding 6.6 years between 2019 and 2021, to 65.2 – equal to the average U.S. life expectancy in 1944.
Reversing the dramatic declines of the past two years will not come easily, even as COVID-related deaths continue to drop. According to Debbie Salas-Lopez, Northwell Health’s senior vice president of community and population health, “we’re not going to catch up anytime soon.”
Wealthier, higher-educated families and individuals will fare better, but Salas-Lopez believes it will take many years for less-educated, economically disadvantaged communities to regain those lost years of life expectancy.
“There’s a link between life expectancy and level of education,” the doctor notes, “just like there’s a link between life expectancy and income earned.”
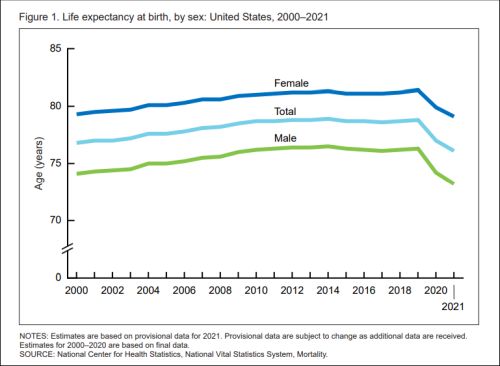
Wrong direction: Average U.S. life expectancies are in dramatic decline.
Among the numerous factors driving down global lifespans are new (and old) viruses that are emerging (and reemerging) in the United States and around the world, as evidenced by COVID and more recently monkeypox. The impacts of climate change are also significant, Salas-Lopez adds, with warmer temperatures reducing air quality and causing destructive storms and wildfires – generating more heat-related illnesses and droughts that are destroying food sources, adding to global hunger concerns.
The U.S. death toll has also been enlarged by other public-health issues, such as gun violence (which killed more than 45,000 Americans last year) and numerous mental-health disorders, ranging from anxiety and depression to PTSD and substance abuse. All of the above contribute to higher suicide rates, among other life-and-death consequences.
Salas-Lopez acknowledges that these problems were all prevalent before these last two difficult years. But the COVID public health emergency, she notes, pushed other concerns into the back seat.

Debbie Salas-Lopez: Mental healthier.
“COVID distracted us,” Salas-Lopez says. “It worsened not only substance abuse, but a lot of other mental-health problems.”
Recognizing that mental-health awareness and access to services are lacking on Long Island, Salas-Lopez convened a Health Equity Task Force for Nassau and Suffolk counties, facilitating COVID vaccinations in underserved communities and working closely with mental-health associations across the Island on a series of day-long mental-health training sessions, set to begin later this month.
The goal, she says, is to educate local community leaders about early warning signs, enabling them to intervene with local residents who may be at risk of a mental-health crisis, and possibly refer them to local behavioral-health service providers for treatment.
Hopefully, some of those spiraling deaths can be prevented and another public health emergency can be avoided. Mental health, according to Salas-Lopez, is “the new pandemic.”
“Community organizing around mental-health resources and providing more education, training and awareness is really going to be the only way to address the underlying problem,” she adds.
Terry Lynam is a communications consultant and former senior vice president/chief public relations officer for Northwell Health.







