By TERRY LYNAM //
Today, Feb. 11, marks the two-year anniversary of COVID-19 – at least, the anniversary of the World Health Organization giving the novel coronavirus a formal name.
 Another noteworthy anniversary is coming on Feb. 26: Two years since the U.S. Centers for Disease Control and Prevention reported the first suspected U.S. case of COVID-19.
Another noteworthy anniversary is coming on Feb. 26: Two years since the U.S. Centers for Disease Control and Prevention reported the first suspected U.S. case of COVID-19.
Reflecting on COVID-19’s two-year anniversary – and the impact it’s had on society and our lives – naturally raises this question: When will we be rid of this virus?
Every time COVID-19 cases wane and it looks like we’re nearing the end of the public health crisis, a new, previously unknown pathogen emerges somewhere on the planet, sure to eventually makes its way to the United States. We saw cases spike when the Delta variant hit our shores in March 2021, and even worse numbers after Omicron struck home in December.
While symptoms associated with the latest variant are not life-threatening for most of those who had been vaccinated, the death rate spiked significantly over the past six weeks among those who were not, particularly older individuals with underlying health conditions. Even as Omicron cases and hospitalizations continue to drop, thousands of Americans are still dying every day.

Terry Lynam: Where do we go from here?
Over the past six weeks, global health experts have reported that Omicron sickened more people at once than anything since the 1917-18 flu pandemic, which killed an estimated 50 million people worldwide. By mid-January, Omicron had sickened 1-in-5 Americans; some think the tallies will double before the surge ends sometime this month.
That raises the next question: What does the future of COVID look like?
David Hirschwerk, an infectious disease specialist recently promoted to medical director of Manhasset’s North Shore University Hospital, Long Island’s largest hospital, believes it’s “highly likely we will see new variants come and go.”
Basically, COVID isn’t going to disappear entirely in the foreseeable future – but the good news, according to Hirschwerk, is the cyclical surges probably won’t be as high as we’ve seen with Omicron, especially as a larger percentage of the national and global populations achieve some degree of protection (either from vaccines or increased exposure, building up herd immunity).
Will we need annual COVID vaccines, similar to flu inoculations? Hirschwerk thinks it’s possible – if not yearly, on some kind of regular schedule. “I envision a situation where at some interval, people are going to need to continue to get vaccinated,” the doctor says. “I’m just not sure what that interval will be.”
Unfortunately, only about 42 percent of the roughly 212 Americans who were previously “fully” vaccinated have come back for boosters, so the prospect of them rolling up their sleeves for ongoing vaccinations is not promising.

David Hirschwerk: No end in sight.
It’s no coincidence that COVID has claimed more lives (upwards of 901,000) in the United States than any other country, when you consider the nation’s vast population and low vaccination rate – just 64 percent of the eligible population, one of the worst rates among developed countries where vaccine supply is not an issue.
Resistance to vaccines, mask-wearing and social distancing are the primary reasons America can’t shake this pandemic, but those opposing public-health guidance tend to complain the loudest about COVID-related restrictions and our inability to “get back to normal.”
The CDC has gotten its fair share of criticism for its communications strategies, but Hirschwerk believes it’s misguided to blame the agency for its handling of the crisis.
“The CDC has had its missteps,” he notes. “But this is a new germ that we only have a limited amount of experience with.”
And the scientific and public-messaging challenges of diagnosing, treating and controlling this new pathogen have been further complicated by the “tension of balancing public safety with the need of society to maintain a certain degree of function,” according to Hirschwerk.
“I’m a firm believer in the mission, value and overall focus of the CDC,” he adds.
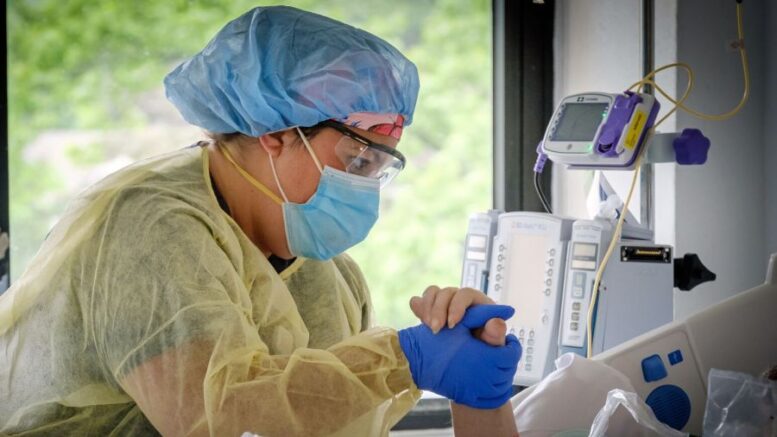
For the exhausted U.S. caregivers who’ve been on the front lines of this crisis for two years, the pandemic’s end cannot come soon enough. While trying to maintain some semblance of family life, they’ve had to deal with the physical and emotional stress of seeing unprecedented numbers of patients die under their care – not to mention many of their own colleagues who’ve succumbed to the virus.
Over the past two years, America’s healthcare workforce has been challenged like no other time in the past century. With COVID’s two-year anniversary upon on, let’s hope the finish line is in sight.
Terry Lynam is a communications consultant and former senior vice president/chief public relations officer for Northwell Health.