By GREGORY ZELLER //
A disturbing and growing trend of the 2020 pandemic sees non-COVID-19 patients in medical distress avoiding hospital emergency rooms – with detrimental, sometimes fatal consequences.
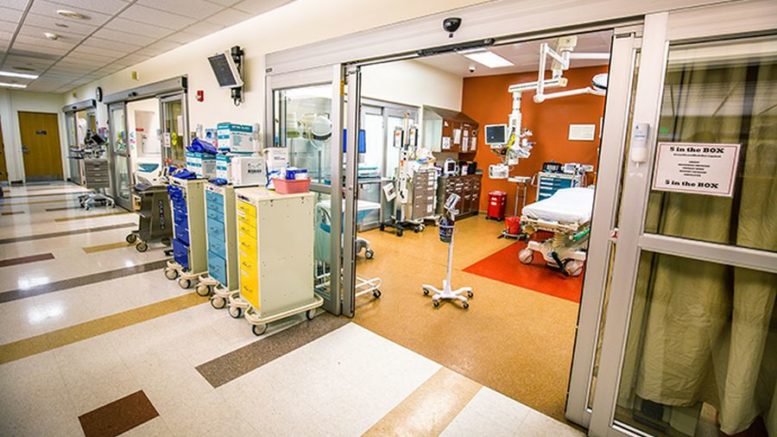
 This dangerous development is evident at Stony Brook University Hospital, where both Emergency Department visits and hospital admissions – minus Persons Under Investigation for the novel coronavirus – are way down.
This dangerous development is evident at Stony Brook University Hospital, where both Emergency Department visits and hospital admissions – minus Persons Under Investigation for the novel coronavirus – are way down.
The lockdowns and quasi-quarantines have myriad effects on emergency room activity; for instance, motor vehicle accidents – a standard of ERs everywhere – are in dramatic decline (various reports say MVAs in New York City, California and other traditionally wreck-heavy regions have been reduced by half or more).
But there is another inescapable conclusion, worrying Stony Brook Medicine and healthcare experts everywhere: Many Americans who need immediate medical attention just aren’t seeking it.

Peter Vicciello: Open for business.
That’s a terrible precedent, according to Peter Viccellio, vice chairman of emergency medicine at Stony Brook University’s Renaissance School of Medicine, who cites sad cases of patients who see COVID-19 as a fate worse than death – and ultimately see that thought through.
“We need to increase public awareness that patients with heart attacks and strokes aren’t coming to the hospital, and they need to,” said Viccellio, a health-policy expert whose areas of research include emergency-department overcrowding and patient safety, among others.
With those and other factors in mind, SBUH has instituted a number of protocols to keep PUIs and non-PUI patients apart and “limit potential exposure in our hospital,” according to Viccellio.
Right at the top: the establishment of a dedicated Emergency Department area, cordoned off by a medical tent, for PUIs to undergo COVID-19 testing.
The hospital has also taken measures to prevent crowding in office and waiting areas and adopted all CDC professional guidelines regarding social distancing and protective equipment, while stepping up sanitization schedules and establishing a new screening system that checks in with non-emergency patients the day before their scheduled hospital visit, and funnels PUIs to coronavirus-designated sections.

Looks bad: Non-PUIs aren’t showing up, even if they need to. (Graph: Stony Brook Medicine)
There’s no doubt SBUH, like hospitals and whole health systems across the country, has been slammed by the pandemic. But specialty groups such as pre- and post-natal care and pediatrics are still on the job, and the hospital remains open to patients with chronic ailments and new health concerns – and, most definitely, life-or-death conditions, according to Stony Brook Medicine Senior Vice President Kenneth Kaushansky.
“While Stony Brook Medicine continues to care for those impacted by COVID-19, it’s important for the community to know that we are still available to meet all their healthcare needs, both in person and online via telemedicine,” Kaushansky, also dean of the Renaissance School of Medicine, said in a statement. “It’s vital for patients with chronic illnesses such as diabetes, heart disease or cancer to continue to seek care from their physicians throughout the Stony Brook Medicine healthcare system.”