By TERRY LYNAM //
At no time in his decade-long tenure has New York Gov. Andrew Cuomo received as much criticism as he and the state Department of Health are getting for withholding data on COVID-related deaths among nursing home patients.
 Lack of full transparency tends to get elected officials in trouble, especially when it involves human lives. The state now concedes that the novel coronavirus killed 15,000 nursing home residents, either in their facilities or in hospitals, a much higher number than previously reported.
Lack of full transparency tends to get elected officials in trouble, especially when it involves human lives. The state now concedes that the novel coronavirus killed 15,000 nursing home residents, either in their facilities or in hospitals, a much higher number than previously reported.
Scrutiny of the governor’s pandemic-related nursing home policies stems from a March 25 Health Department advisory directing nursing homes to accept COVID patients after their discharge from hospitals. The directive was vacated less than two months later as deaths among residents of long-term care facilities spiked and concerns rose that the DOH’s guidance may have contributed to the virus’ spread among an elderly population that was more vulnerable to infection.
While New York State Attorney General Letitia James had already launched an investigation into nursing homes’ responses to the COVID pandemic – and the Cuomo administration’s undercounting of nursing home deaths – the U.S. Department of Justice is now investigating the matter. And state legislators on both sides of the political aisle are considering limiting the governor’s emergency authorization powers.
One year after the coronavirus tightened its deadly grip on New York and the nation, the hunt is on for someone to blame for the tragic deaths among nursing home patients.

Lynam: Blame game.
Setting aside the latest questions of why the state did not disclose the mortality numbers earlier – and whether the Cuomo administration was seeking to avoid a politically motivated investigation by President Trump’s DOJ – recent news coverage of the controversy has included scant mention of the unprecedented crisis that hospitals in the city and on Long Island faced last spring, when New York was the pandemic epicenter.
Most hospitals in eastern Queens and western Nassau County were at or well over capacity during March and April. Thousands of critically ill patients were arriving in growing numbers, every day, forcing local hospitals to create makeshift intensive care units wherever they could find space. Worse was the uncertainty over how long the surge would last.
Not knowing the answer, hospitals put beds in lobbies, conference rooms and other non-traditional areas. Some pitched tents to serve as field units. Staffers were stretched to the limit as hundreds of caregivers contracted the virus, prompting hospitals to bring in out-of-town providers to help with the onslaught.
The stark reality of the daily heartbreak occurring inside hospitals was underscored outside by the presence of refrigerated trailers – makeshift morgues for the growing number of victims.
Most striking to caregivers was the sheer number of critically ill patients. At the height of the pandemic on April 7, Northwell Health hospitals housed 3,425 COVID patients. On average, 26 percent required intensive care and 22 percent were on life support, while 80 to 90 perished each day.
Hospitals understandably were looking to free up beds and discharge patients as quickly as safely possible. The challenge was that many – particularly older, frailer patients – were too sick to go home, required ongoing care and/or lacked a capable caregiver outside the hospital. Temporary field hospitals, like the one established off Manhattan on the U.S. Navy ship USNS Comfort, weren’t allowed to care for those patients.
For most, a nursing home was one of the few available options.
Another important fact that’s been largely overlooked is that the majority of COVID patients being discharged from hospitals may have still tested positive for the virus – but based on criteria from the U.S. Centers for Disease Control and Prevention, most were no longer considered contagious.
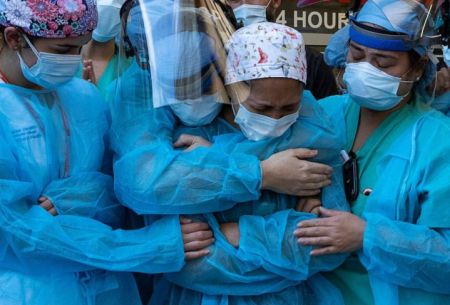
Unprecedented: The pandemic overwhelmed governments and healthcare providers alike.
The bottom line is that there were many factors that contributed to the high number of deaths among nursing home patients. As AG James pointed out in her report last month, many nursing homes lacked compliance with infection-control protocols, had less staff than they did pre-pandemic, had insufficient PPE for staff and lacked adequate access to COVID testing for staff and residents.
Among other thing, the illness highlighted the importance of skilled-nursing facilities as part of our nation’s care continuum – moving forward, we must support nursing home-based caregivers to the same extent as those working in hospitals.
The lessons of the past year and the rapid development of vaccines have also taught us how to prevent and better treat the virus. Sadly, these advances won’t bring back the half-million Americans lost. And understandably, many grieving families are angry and looking for answers.
Given his visibility over the past year, Cuomo may be a convenient scapegoat for this tragedy. But the coronavirus was a disease that we had never seen or treated. And we were not entirely sure how it was transmitted, even as it was spread rapidly through the entire population by asymptomatic carriers.
My guess is that an objective investigation of the governor’s actions will conclude that the unprecedented nature of this virus simply overwhelmed parts of our care delivery system. COVID is not going away anytime soon; it likely will be with us for years to come, much like the seasonal flu. But unlike those darkest days of 2020, we are now much better prepared – on every level.
Terry Lynam is a communications consultant and former senior vice president/chief public relations officer for Northwell Health.








In the words of former President Dwight D. Eisenhower, “The search for a scapegoat is the easiest of all hunting expeditions.” The reality is that Governor Andrew Cuomo provided real leadership at a time when the federal government was in Covid denial. Excellent analysis , Terry.