By TERRY LYNAM //
Keeping track of the Trump Administration’s head-spinning budget cuts and layoffs has been tough, but one thing is clear: They could have a staggering impact on your health.
 Government-sponsored health insurance, scientific research and healthcare providers – especially financially distressed hospitals – are all on the line. Consider one of the administration’s latest bombshells: Eighty thousand federal workers within the U.S. Department of Health & Human Services got an email March 7 offering them buyouts of up to $25,000, including employees responsible for disease research, food inspections, the administration of both Medicaid and Medicare and much more.
Government-sponsored health insurance, scientific research and healthcare providers – especially financially distressed hospitals – are all on the line. Consider one of the administration’s latest bombshells: Eighty thousand federal workers within the U.S. Department of Health & Human Services got an email March 7 offering them buyouts of up to $25,000, including employees responsible for disease research, food inspections, the administration of both Medicaid and Medicare and much more.
The missive gave employees one week to respond. Left unsaid: How many of them will get layoff notices if they don’t take the “voluntary separation incentive,” raising huge questions about who will remain to perform the work of 100-plus HHS programs.
With an annual budget of $1.8 trillion this fiscal year, HHS is the largest federal agency, touching the lives of more Americans than any other department, from newborns to the elderly. Medicaid and Medicare alone have nearly 150 million enrollees. In addition to the Centers for Medicare & Medicaid Services, HHS controls 21 sub-agencies, including the U.S. Centers for Disease Control and Prevention, the U.S. Food and Drug Administration and the National Institutes of Health.

Terry Lynam: Health-scare.
Despite the looming workforce reductions, the Trump Administration has promised an aggressive health and human services agenda. At the urging of HHS Secretary Robert F. Kennedy Jr., President Trump has already signed an executive order creating the Make American Healthy Again Commission, which will focus on “lowering chronic disease rates and ending childhood chronic disease” by pursuing “fresh thinking on nutrition, physical activity, healthy lifestyles, overreliance on medication and treatments, the effects of new technological habits, environmental impacts, and food and drug quality and safety.”
While they support the focus on good nutrition and healthy lifestyles, public health officials have been fretting for months about Kennedy’s vaccine skepticism. Already rattled by recent measles outbreaks in Texas and New Mexico, scientists were deeply concerned by the news last week that the CDC is preparing to conduct a large-scale study on whether there is a connection between vaccines and autism, despite dozens of previous studies that found no evidence of a link.
Healthcare leaders are also sounding alarms about pending Medicaid cuts. To meet the budget targets needed to pass President Trump’s legislative agenda, Congressional Republicans have directed the committee that oversees Medicaid and Medicare to cut $880 billion over the next decade.
Given Trump’s promise not to mess with Medicare, it’s expected that the vast majority of the cuts will target Medicaid, which provides health coverage to about 79 million low-income and disabled adults and children, including nearly two-thirds of the nation’s nursing home residents.
 The federal government currently pays about 69 percent of Medicaid costs, with states and local governments picking up the rest. Twenty-six states require counties to help pay for their share of Medicaid. In New York, 57 counties and the City of New York are shelling out $8.5 billion this fiscal year toward the state’s Medicaid program – the largest local share in the country.
The federal government currently pays about 69 percent of Medicaid costs, with states and local governments picking up the rest. Twenty-six states require counties to help pay for their share of Medicaid. In New York, 57 counties and the City of New York are shelling out $8.5 billion this fiscal year toward the state’s Medicaid program – the largest local share in the country.
The financial burden on states and localities will get even heavier as Congressional Republicans look to lower the federal government’s share of Medicaid costs. In response, states would need to make tough choices, including whether to discontinue Medicaid coverage to 20 million Americans who qualify for expanded eligibility through the Affordable Care Act, a.k.a. Obamacare.
The ACA enables all adults with incomes up to 138 percent of the federal poverty level ($21,597 for individuals and $44,367 for a family of four) to access ACA subsidies and provides states with more federal money for expanding insurance access. Forty states (including New York) and the District of Columbia took advantage by expanding Medicaid eligibility, but 12 of those states have laws on the books that will automatically cut coverage for those higher-income Obamacare recipients if the federal match drops.
Considering the financial burden, other states may also be forced to discontinue coverage for those enrollees or reduce optional benefits such as prescription drug coverage.
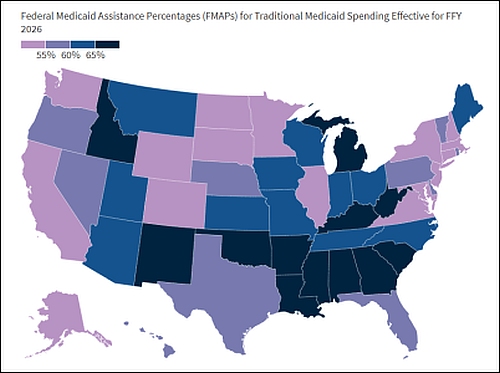
Show me where it hurts: Lower-income states receive the lion’s share of federal Medicaid assistance — and will feel pending funding cuts the most. (Source: Kaiser Family Foundation)
States’ reliance on Medicaid dollars is so great that, even if they reduce eligibility, they might still need to raise taxes or make significant cuts elsewhere to make up for the lost federal revenue. In New York, Medicaid spending reaches $101.5 billion in the current fiscal year, with the federal government paying $57 billion, the state covering nearly $36 billion and local governments picking up the rest.
New York’s healthcare leaders are bracing for the worst. They’re warning that the impact could be catastrophic on safety-net hospitals and nursing homes that serve low-income populations and rely heavily on Medicaid funding.
On Long Island, healthcare leaders and local state legislators are fighting to keep Nassau University Medical Center afloat by pressuring Gov. Kathy Hochul and the State Legislature for more state funding.
The severity of the budget pain will be determined in the coming months. But if hospitals close, millions of Americans lose their health insurance and public health is threatened, Congressional Republicans in swing districts could feel some pain of their own in next year’s midterm elections.
Terry Lynam is a communications consultant and former senior vice president/chief public relations officer for Northwell Health.