By GREGORY ZELLER //
The Feinstein Institutes for Medical Research has begun an ambitious mapping mission that may chart the course to the human race’s healthiest future.
 A $6.7 million National Institutes of Health award will fund the creation of a detailed anatomical map of the human vagus nerve, a parasympathetic superhighway to and from the brain responsible for everything from our heart rate to our inflammatory/immune response the breaths we take.
A $6.7 million National Institutes of Health award will fund the creation of a detailed anatomical map of the human vagus nerve, a parasympathetic superhighway to and from the brain responsible for everything from our heart rate to our inflammatory/immune response the breaths we take.
Known officially as REVA (for “Reconstructing Vagal Anatomy”), the first-of-its-kind mapping will be “down to each and every sensory and motor fiber,” according to Northwell Health’s Manhasset-based R&D mothership, and that’s saying something: The vagus nerve – which runs from the brainstem to vital organs in the neck, chest and abdomen – is comprised of 100,000 individual fibers, grouped into bundles called “fascicles.”
The detailed breakdown – including high-definition 3D tomographic imaging and a new “microanatomy atlas,” among other data – will mark an exponential leap for bioelectronic medicine, the field focused on electrical nerve stimulation as a drug-free treatment for inflammatory diseases and other conditions.

Stavros Zanos: Accurate characterization.
Of course, it’s also right in the wheelhouse of the bioelectronics-heavy Feinstein Institutes and its stable of world-renowned bioelectronics experts, including President/CEO Kevin Tracey and Institute of Bioelectronic Medicine Associate Professor Stavros Zanos, who’s leading the three-year mapping effort.
Science already knows the vagus nerve continuously conveys information between the brain and the body, thereby facilitating basic physiological functions – but “how sensory and motor fibers are arranged inside the vagus nerve and pathways to different organs [is] essentially unknown,” according to Zanos.
Enter REVA, which will finally chart that course.
“With the support of the NIH, we hope to characterize the nerve’s microscopic structure so that we better understand its function in health and disease,” Zanos added. “[This] will ultimately lead to new ways to treat disease with bioelectronic devices through vagus nerve stimulation.”
The mapping effort will dissect 60 nerves collected from 30 human cadavers. Artificial intelligence protocols will help correlate and analyze the collected data, ultimately helping Zanos and his team create a map of what the Feinstein Institutes called “unprecedented detail,” for use by global researchers.
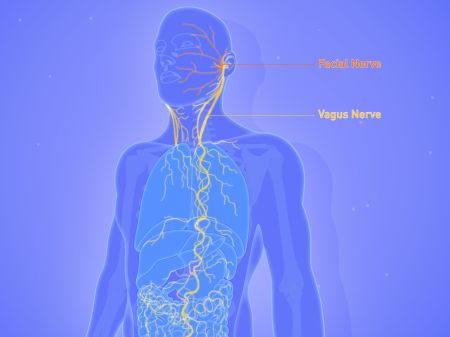
Details to follow: Expect future vagus-nerve maps to be a little more comprehensive.
That team includes Zanos’ brother, Institute of Bioelectronic Medicine Associate Professor Theodoros Zanos; Feinstein Institutes Professor Larry Miller, who pulls double duty in the Bioelectronics Medicine and Health Innovations & Outcomes Research institutes; Zucker School of Medicine at Hofstra/Northwell Assistant Professor of Science Education Zeinab Nassrallah; and Mary Barbe, professor of cardiovascular sciences at Temple University’s Lewis Katz School of Medicine.
It’s an impressive lineup worthy of the chunky NIH investment and the immense scientific challenge, according to Tracey, the preeminent bioelectronics pioneer at the Feinstein Institutes’ helm, who considers the research a big step toward “cur[ing] disease with bioelectronic devices.”
“The vagus nerve … can turn on and off our immune system,” the CEO said in a statement. “This research … generates fundamental new knowledge that will transform our understanding of the human vagus nerve and open new ways to hack the vagus nerve.”