By TERRY LYNAM //
For many, trust in the family doctor runs deep – we routinely turn to them first, whenever we’re sick or concerned about symptoms that might signal a larger health issue.
 They may have our confidence, but more than seven in 10 U.S. primary-care physicians now work for insurance companies, private-equity firms, health systems or hospitals. This inevitably raises questions about their decisions – are they influenced by the patient’s best interests or their employer’s profit margins?
They may have our confidence, but more than seven in 10 U.S. primary-care physicians now work for insurance companies, private-equity firms, health systems or hospitals. This inevitably raises questions about their decisions – are they influenced by the patient’s best interests or their employer’s profit margins?
Critics refer to this as the Medical Industrial Complex, a rising phenomenon in which a growing number of for-profit conglomerates manage healthcare for hundreds of millions of Americans.
Practices employing the nation’s approximately 268,000 primary-care physicians – historically overworked and underpaid, compared to peers in other medical specialties – have become prime acquisition targets, especially for commercial insurers and private-equity firms that invest billions of dollars annually to control healthcare’s consumer front door.
In 2010, private investment in primary care amounted to $15 million. Last year alone, CVS Health – owners of insurance giant Aetna – laid out $10.6 billion to buy Oak Street Health and the 600 primary-care providers it employs across 169 medical centers in 21 states. Amazon, meanwhile, paid $3.9 billion to purchase One Medical, a primary-care practice with nearly 200 locations serving more than 836,000 patients.
Not to be outdone, the nation’s largest health insurer, UnitedHealth Group, now employs or contracts with more than 90,000 physicians (and 40,000 other clinicians) through its subsidiary Optum Inc. Optum has more than doubled in size over the past four years, with 2,200 nationwide locations (including dozens on Long Island) and $226 billion in 2023 annual revenue – a 24 percent jump from 2022.

Terry Lynam: Still trust the family doctor?
So, what’s the attraction? They may be one of medicine’s less-lucrative specialties, but the nation’s primary-care practices log 400 million-plus patient visits annually, generating enormous downstream revenue for insurers, hospital systems, pharmacies and others with a financial stake in healthcare.
Another big allure is the increased privatization of Medicare, the federal health insurance program covering more than 65 million Americans ages 65 and over. Primary-care doctors treat many of the 31 million people enrolled in Medicare Advantage plans offered by private insurance companies, to whom the federal government pays more than $400 billion annually to cover enrollees.
Based on a patient’s health history, Medicare allocates a fixed amount to commercial insurers and providers for managing the health of each Medicare Advantage enrollee. That’s an incentive to keep patients healthy and out of the hospital, largely through preventive care.
Patients are attracted to Medicare Advantage plans because they’re considerably cheaper than traditional Medicare (though they usually require patients to use in-network providers and get specialist referrals). Insurers like MA’s so-called “value-based” approach, because it keeps down costs, enabling physician practices that take on the financial risk of patient care to share profits with insurers.
Medicare Advantage’s spiraling burden on the federal government has watchdogs, however, and they’re calling for reforms – accusing insurers of gaming the system by enrolling healthier, lower-cost customers and using aggressive coding to exaggerate patients’ health risks (a path to higher Medicare payments).
A report issued earlier this month by Congress’ nonpartisan Medicare Payment Advisory Commission estimated that the federal government could pay MA plans $88 billion more this year than it would be spending if those seniors were enrolled in traditional Medicare.
There are more than 8,000 different MA plans available to retirees nationwide this year, but large insurers have a stranglehold on the market. UnitedHealthcare and Humana account for nearly 47 percent of all enrollees.
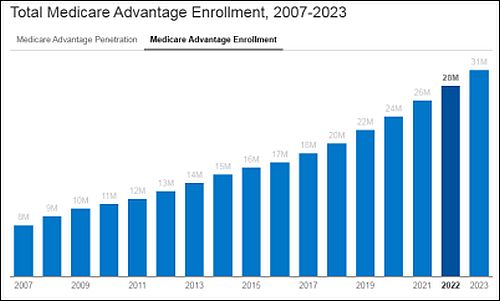
Up and up: Nationwide enrollment in Medicare Advantage programs is soaring … and government expenditures are rising along with them. (Source: KFF)
Whether it’s insurers, providers, pharmacies or other healthcare entities, scale is the differentiator in today’s $4.5 trillion healthcare market, which is why investors have swooped in.
Far beyond primary-care practices, private equity investors are assuming ownership of large parts of the U.S. healthcare system. Over the past decade, private equity firms have spent nearly $1 trillion to purchase hospitals and specialized medical practices, according to a 2022 investigation by Kaiser Health News.
The ultimate question is: How will the rising tide of corporate medicine impact consumers?
Will it increase healthcare and insurance costs even more? Change the sacred doctor-patient relationship? Will conglomerates that control physician practices restrict the services patients can access, including hospital care?
Insiders can debate the merits and ethics of for-profit vs. nonprofit healthcare. Many argue that both can be equally cutthroat. But no matter whose name is on their paycheck, doctors continue to have a basic obligation: Keep the best interests of patients front and center.
Terry Lynam is a communications consultant and former senior vice president/chief public relations officer for Northwell Health.